Toxocara larvae, mostly of the species T. canis and T. cati, can infest human hosts to cause various clinical manifestations. These include visceral and ocular larva migrans. Ocular larva migrans is a debilitating condition which can cause vision loss in children. For this reason, this relatively rare condition requires to be diagnosed and treated adequately.
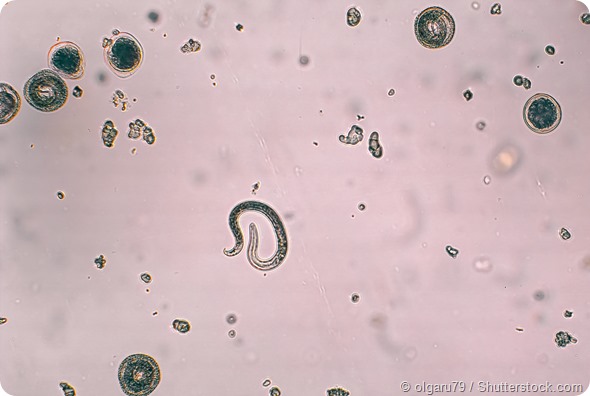
Toxocara canis and embryonated egg with larva.
Diagnosis
The ocular manifestations of toxocara larva infestation are varied.
Children with toxocarial ocular larva migrans are mostly asymptomatic. In a few cases, they may have the clinical features of covert toxocariasis or visceral larva migrans. The major risk factors are contact with dogs and cats, especially puppies and kittens which have a higher rate of infestation with Toxocara.
In the majority of cases (90%), ocular larva migrans affects only one eye. Most children with ocular larva migrans are in the age group of 3-11 years, though recently the incidence among young teenagers has been reported to be higher. The most common symptoms include:
- Blindness of one eye: this is reported by over 80% of patients, and is permanent in most cases
- Floaters in almost 40%
- Bloodshot conjunctiva in a third of cases
- Photophobia in a third of patients
- Ocular pain in a fifth of affected children
- Leukocoria or white pupillary reflex
- Vitreous inflammation
- Squinting
In some children the retinal symptoms may be associated with those due to central nervous system infestation.
On examination, the affected eye shows features such as:
- Granulomas of the subretinal space in 65%
- Visual field scotomata in half the patients
- Vitreous inflammation in over half of cases
- Posterior pole granulomas in over 40%
- Peripheral granulomas with traction bands in almost 40%
- Chorioretinal inflammation in one-third of patients, resolving to form a well-defined whitish lesion with retinal folds and disturbed retinal pigment epithelium
- Retinal detachment in more than a quarter of cases, often peripapillary and associated with optic disc granulomas
- Strabismus in over a quarter
- Inflammation of the anterior uvea in a quarter
- Leukocoria in 15%
- Endophthalmitis, often with strangely muted symptoms but vivid signs on examination
Visual loss in cases of OLM is due to the morbidity caused by:
- Retinitis
- Vitreous inflammation
- Cystoid macular edema
- Cataract formation
- Retinal detachment
- Neovascular membrane formation
- Macular detachment due to traction
- Amblyopia due to opacities and macular involvement
- Optic nerve head atrophy in a few cases
Fundoscopy and visual field examination should be supplemented by serologic tests and histopathology, if a surgical specimen is available, to examine any larvae obtained from the tissue. The potential risk of surgery in such cases has led to newer immunologic tests being developed.
Optical coherence tomography (OCT) shows highly reflective masses above the retinal pigment epithelium layer, when posterior pole granulomas are present. In addition, risk factors for retinal detachment may be detected.
Treatment
Treatment is primarily medical and is focused on preventing damage and visual loss due to the inflammatory reaction in the eye caused by the presence of the larva and the formation of secondary membranes. The first drug of choice is a potent glucocorticoid which can suppress local inflammation, stabilize cell membranes and reduce the release of local mediators of allergy and inflammation.
Either topical steroids are used or they are infiltrated into the periocular space. Intraocular or systemic steroids may also be useful depending on the clinical situation.
Treatment with antihelminthic medications is used when there is evidence of continuing infestation elsewhere in the body. The most commonly used drugs include albendazole, which has larvicidal activity and can penetrate the blood-brain barrier, as well as diethylcarbamazine. Quiescent infection should not be treated because of the danger of inflammation from a dying or dead worm.
Surgical methods are useful in treating some cases with vitreous bands, scars or retinal detachment. Laser photocoagulation of larvae, cryosurgery or surgical vitrectomy have all been recommended in various situations.
Uveitis following toxocara ocular infestation responds well to antihelminthics and corticosteroids but vision, unfortunately, is often permanently damaged or lost. In most cases the damage to the ocular structures is irreversible. Whatever the mode of treatment, the visual outcome cannot be expected to be completely satisfactory, in most cases.
References
- http://link.springer.com/article/10.1007/s40475-013-0004-5
- https://www.reviewofophthalmology.com/article/detection-and-treatment-of-ocular-toxocariasis
Further Reading
Last Updated: Feb 27, 2019