Introduction
Topical agents for the treatment of scabies
Oral agents for the treatment of scabies
References
Scabies is a major global health problem caused by the mite Sarcoptes scabiei var. hominis, an obligate human ectoparasite measuring between 330 and 450 µm in length. Treatment of this disease has undergone various changes since the days of Roman physician Celsus when sulfur mixed with liquid pitch was used as a primary approach.
Today, scabies therapy involves making the precise diagnosis, identifying the correct clinical context to guide treatment of contacts and fomites, selecting the most effective medication, understanding how to use the agent appropriately, and following a rational basis for when to use and reuse a drug of choice. Scabicidal drugs can be broadly divided into topical agents and oral agents.
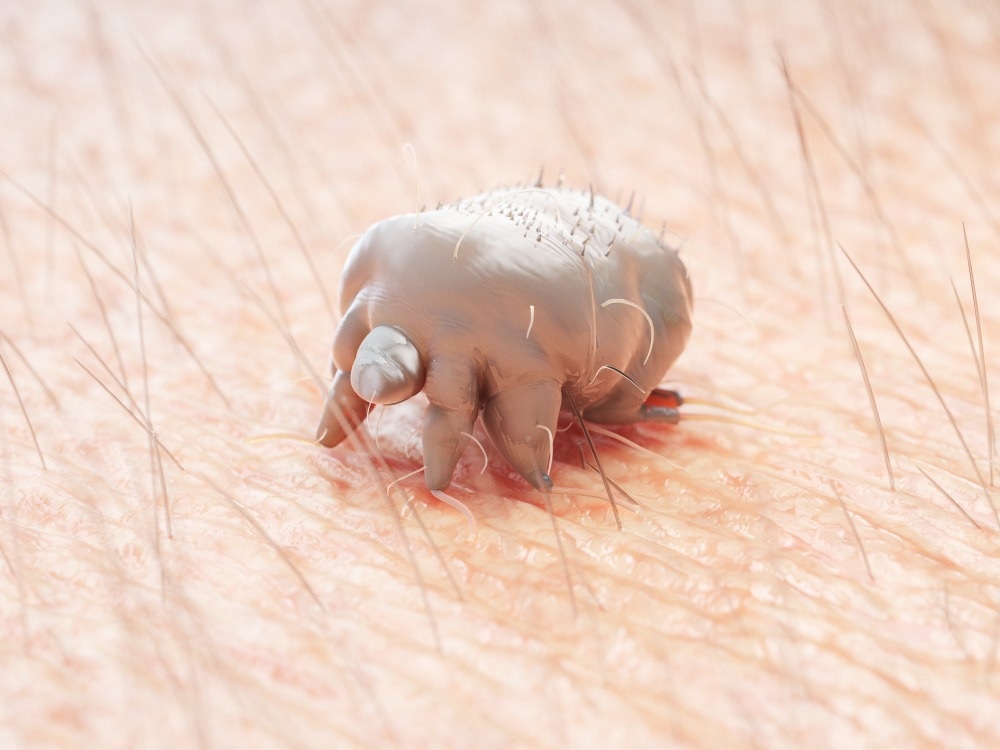
Image Credit: SciePro/Shutterstock.com
Topical agents for the treatment of scabies
The mainstay of scabies treatment are topical scabicidal agents. Permethrin 5% cream is currently accepted as the gold standard because of an efficacy greater than 90% and excellent safety profile. This topical drug is labeled for application to the entire body for 8 to 12 hours, usually right before bedtime.
Lindane 1% cream or lotion (also known as gamma benzene hexachloride) has been found to be an effective alternative option in treating this ectoparasitosis. Nevertheless, its potential neurotoxicity (especially with repeated applications) has limited its use; thus, the product is no longer available in certain countries.
Benzyl benzoate, an ester of benzoic acid and benzyl alcohol, is neurotoxic to the mites and is used as a 25% emulsion for the contact period of 24 hours. As it is very effective when used properly, the emulsion should be applied below the neck three times within 24 hours without an intervening bath. Its use increased for the treatment of permethrin-resistant crusted scabies.
Crotamiton is used as 10% cream or lotion with a success rate between 50% and 70%, significantly less effective than permethrin. Although this topical agent is labeled for application over 1 to 2 days, daily application for 5 days has yielded improved cure rates.
The effectiveness of malathion 0.5% lotion has been demonstrated by several small studies, with cure rates ranging from 83% to 100%. It is appropriate for treating hairy areas of the body (such as the scalp) and requires two applications 7 days apart.
As increasing resistance to scabies treatments may be on the horizon, the standard of care should encompass routine treatment of the scalp and face and re-treatment of patients at day 4 (based on the scabies life cycle) to guarantee more efficient mite eradication. Furthermore, practitioners should attempt to treat all close contacts concurrently with the source patient.
Image Credit: Mykola Samoilenko/Shutterstock.com
Oral agents for the treatment of scabies
Oral Ivermectin, a drug initially used in humans to control outbreaks of onchocerciasis in Africa and Latin America, can now be used as an off-label oral medication for scabies (alone or in combination with a topical agent). Most studies have shown that one or two doses of Ivermectin (200 µg per kilogram of body weight) result in cure rates equivalent to treatment with conventional topical medications.
Efficacy rates from open-label studies of Ivermectin for treating classic scabies range from 76% to 100%. The drug's safety profile is also considered good, as no serious adverse effects were noted in the treatment of a large number of children with scabies in the Solomon Islands.
There is some observational evidence of Ivermectin's effectiveness in controlling scabies outbreaks in institutional settings such as nursing homes. Mass drug administration programs have attempted to use this agent for scabies control in endemic communities around the world; however, such programs' superiority over alternative topical treatments is questionable.
Populations must be educated and sensitized on related preventive measures such as adopting rigorous personal hygiene, avoiding overcrowding and overpopulation in rooms and houses whenever possible, and promoting or reinforcing hand hygiene.
References:
- United Kingdom National Guideline on the Management of Scabies infestation (2007) Clinical Effectiveness Group (British Association of Sexual Health and HIV) Introduction and methodology. (n.d.). [online] Available at: https://www.bashh.org/documents/27/27.pdf [Accessed 1 Aug. 2022].
- Walton, S.F. and Currie, B.J. (2007). Problems in Diagnosing Scabies, a Global Disease in Human and Animal Populations. Clinical Microbiology Reviews, [online] 20(2), pp.268–279. doi:10.1128/CMR.00042-06.
- Johnstone, P. and Strong, M. (2009). Scabies. American Family Physician, [online] 79(12), pp.1089–1090. Available at: https://www.aafp.org/pubs/afp/issues/2009/0615/p1089.html [Accessed 1 Aug. 2022].
- Thomas, J., Peterson, G.M., Walton, S.F. et al. Scabies: an ancient global disease with a need for new therapies. BMC Infect Dis 15, 250 (2015). https://doi.org/10.1186/s12879-015-0983-z
- Chosidow, O. (2006). Clinical practices. Scabies. The New England Journal of Medicine, [online] 354(16), pp.1718–1727. doi:10.1056/NEJMcp052784.
- Albakri L, Goldman RD. Permethrin for scabies in children. Can Fam Physician. 2010 Oct;56(10):1005-6. PMID: 20944041; PMCID: PMC2954078.
- American Academy of Pediatrics. Scabies. In: Pickering LK, Baker CJ, Kimberlin DW, Long SS, editors. Red Book: 2009 Report of the Committee on Infectious Diseases, 28th ed. Elk Grove Village, IL: American Academy of Pediatrics, 2009; pp. 589-591.
Further Reading
Last Updated: Aug 10, 2022