Migraine is a condition associated with painful headaches. It is a neurological disorder that can significantly impact an individual's quality of daily life. Although the global prevalence of migraine is high, this condition is under-recognized and undertreated. Typically, people younger than 50 years of age are affected by this recurrent neurological disorder. Migraine also leads to substantial economic losses, both directly and indirectly.
Several gastrointestinal symptoms, such as diarrhea, constipation, vomiting, nausea, and dyspepsia, are associated with migraine. Furthermore, this neurological condition has been linked with the development of irritable bowel syndrome and inflammatory bowel disease (IBD). These findings suggest that migraine could be connected to the interplay of the gut–brain axis.
IBD comprises two chronic inflammatory gastrointestinal disorders, namely, Crohn's disease (CD) and ulcerative colitis (UC). Many studies have identified the generic and environmental factors that increase the risk of IBD. These studies have also determined the modifiable risk factors that prevent the onset of IBD. In comparison to the general public, IBD patients are at a higher risk of migraine. To date, no studies have investigated whether migraine impacts the development of IBD.
About the Study
The current study evaluated the association between migraine and IBD manifestation using a nationwide cohort. This study obtained data from the National Health Insurance Service (NHIS), the nationwide healthcare system for South Korean citizens. This database includes detailed demographic and medical information on both outpatients and inpatients.
Individuals who attended the routine health screenings organized by NHIS between January 2009 and December 2009 were recruited, and those with missing data were excluded.
Study Findings
A total of 10,131,193 individuals were recruited as per the eligibility. Around 2.8% of the study population were affected with IBD. Compared to the control group, seniors, females, low-income individuals, and those who resided in rural settings were more likely to have migraine. Furthermore, migraineurs were at a higher risk of developing IBD by 1.3-fold, compared to the general public.
Consistent with the findings of the present study, previous studies indicated IBD to be an independent factor of migraine disorder. However, this observation was contradicted by a cross-sectional UK Biobank study, which stated IBD was not associated with migraine.
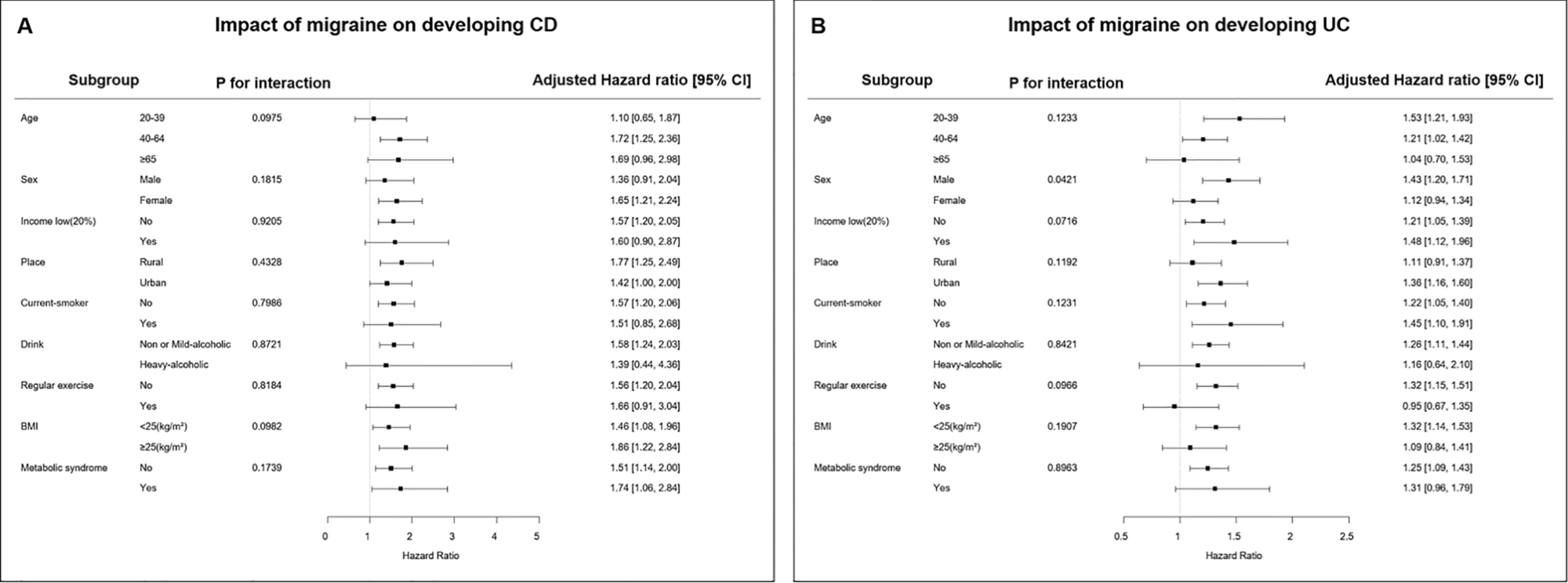 Subgroup analysis for the risk of (A) Crohn’s disease and (B) ulcerative colitis in patents with migraine compared to control groups.
Subgroup analysis for the risk of (A) Crohn’s disease and (B) ulcerative colitis in patents with migraine compared to control groups.
A higher number of participants with migraine were associated with diseases such as chronic kidney disease (CKD), hypertension (HTN), and dyslipidemia. This observation was consistent with previous studies that documented an increased risk of metabolic syndrome and cardiovascular disease in IBD patients.
The sub-group analysis indicated a higher risk of developing IBD, i.e., both CD and UC, in patients with migraine, compared to the general population. After migraine diagnosis, patients were found to be at a higher risk of developing CD. Interestingly, a significant surge in CD diagnosis was observed after five years of follow-up among migraineurs. The risk of CD development among migraineurs was not affected by sex, age, metabolic comorbidities, or health behavior. In contrast, a significant association was observed in male UC patients.
Although regular screening for migraine in clinical settings is not possible, IBD-related awareness could be increased, which could enable early diagnosis and treatment for the same. Previous studies have identified multiple mechanisms that connect migration with the development of IBD. For instance, the development of proinflammatory cytokines, such as tumor necrosis factor-α and interleukin (IL)-1b, were linked with migraine pain. A spike in proinflammatory cytokines levels causes migraine attacks, which are also linked with IBD pathogenesis. Gut microbial dysbiosis is another factor associated with the pathophysiology of IBD and migraines.
Dietary habits, particularly the Western diet, can instigate the development of migraine in episodic or chronic forms. Several studies have also shown that this diet type leads to the development of IBD. Citrus fruit, gluten, coffee, alcoholic beverages, and chocolate are dietary risk factors for both IBD and migraine.
Pharmaceutical agents, such as nonsteroidal anti-inflammatory drugs (NSAIDs), used to alleviate migraine symptoms could trigger the development of IBD. A higher frequency of NSAID intervention increases the risk of CD development.
Conclusions
Due to the lack of appropriate data, this study has some limitations, including its inability to determine how the severity of migraine and IBD are linked. In addition, this study did not consider important covariates, such as dietary patterns, healthcare, stress, family history of IBD, and other gastrointestinal disorders.
Despite the limitations, the current study revealed that migraine is a significant risk factor for IBD development. Using a nationwide study cohort and a long follow-up period are two key strengths of this study. Considering the findings that stated patients with migraine are at a higher risk of IBD, clinicians must explore the gut–brain axis further to better understand how IBD development and migraine are associated.